Encuentre respuestas reales

Un diagnóstico de la enfermedad de Parkinson (EP) suele ir acompañado de una interminable lista de preguntas. Preguntas que evolucionan al ritmo de la enfermedad y de su capacidad para afrontarla. Este mes de abril, con motivo del Mes de la Concientización sobre el Parkinson, queremos ayudar a las personas a encontrar respuestas reales cuando se trata del Parkinson.
Cuando el Parkinson se vuelve real, la Parkinson's Foundation está para ayudarle a encontrar respuestas reales. Ofrecemos asistencia confiable y accesible a través de nuestra Línea de Ayuda, nuestro sitio web, las redes sociales y nuestra nueva función de chat con inteligencia artificial (IA): Ask PAM (pregúntele a PAM).
Estas son algunas de las preguntas y respuestas más frecuentes que hacen las personas sobre el Parkinson:
¿Cuáles son los signos tempranos del Parkinson?
Los primeros signos del Parkinson pueden ser sutiles. Si bien los síntomas motores, como temblores, rigidez y problemas de equilibrio, son los más evidentes, los primeros signos también incluyen cambios en la escritura, pérdida del olfato, problemas para dormir y vértigo. Conozca los 10 signos tempranos de la EP.
¿Qué hacer cuando se notan los primeros signos?
Ningún síntoma por sí solo significa que tenga Parkinson. Si tiene varios síntomas, considere ver a su médico de cabecera y, luego, pedir que lo mande a un neurólogo o, en el mejor de los casos, a un especialista en trastornos del movimiento (un neurólogo especializado). Siga leyendo sobre este tema.
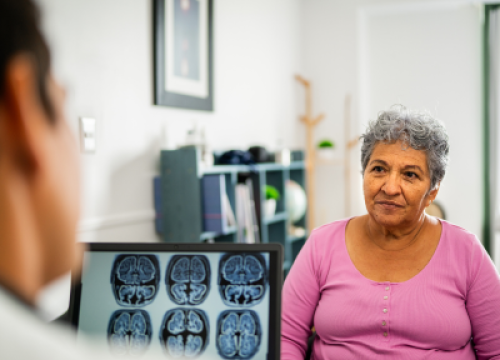
¿Cómo se diagnostica el Parkinson?
El diagnóstico del Parkinson se basa en la observación: el doctor evalúa el historial médico, los síntomas actuales y un examen físico. Ningún laboratorio o prueba por sí solo confirma un diagnóstico, aunque ciertas pruebas pueden ayudar a descartar otras afecciones. Aprenda más acerca del diagnóstico.
¿Qué causa el Parkinson?
Los científicos creen que la causa del Parkinson es una combinación de factores genéticos y ambientales. La genética contribuye a un 10-15% de los casos de la EP, con mutaciones genéticas específicas vinculadas a la enfermedad. Aprenda más acerca de este tema.
¡Ponga a prueba sus conocimientos sobre la EP ahora!

¿Cómo se manejan los síntomas del Parkinson?
Los síntomas más evidentes de la EP se llaman síntomas motores. El Parkinson se llama trastorno del movimiento porque provoca temblores, movimientos lentos y rigidez muscular. Sin embargo, los síntomas no motores son frecuentes y pueden ser más molestos e incapacitantes que los síntomas motores para muchas personas con Parkinson. Éstos pueden incluir depresión, ansiedad, problemas de sueño y más.
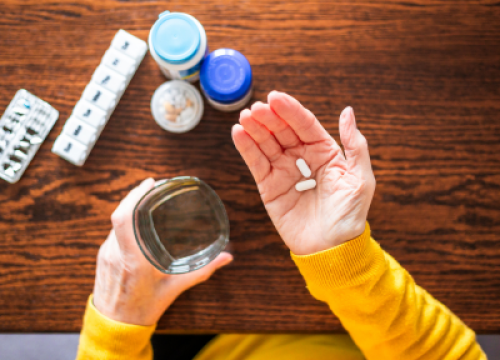
El tratamiento suele incluir medicamentos específicos para sus necesidades. El medicamento Levodopa es el tratamiento más eficaz para los síntomas motores, ya que se convierte en dopamina en el cerebro. Los tratamientos también incluyen cosas que puede hacer usted mismo, como ejercicio y terapias de rehabilitación, como fisioterapia o terapia del habla y el lenguaje.
¿Existe una cura para el Parkinson?
Aunque el Parkinson no tiene cura, los tratamientos pueden manejar eficazmente los síntomas. Los medicamentos, el ejercicio y las terapias de rehabilitación ayudan a mantener la movilidad, el equilibrio y la salud mental. La Parkinson's Foundation también financia la investigación para impulsar mejores tratamientos y acercarnos a una cura. Explorar la investigación actual sobre la EP.
¿Se puede vivir mucho tiempo con Parkinson?
Sí. Los síntomas y el ritmo de progresión del Parkinson son únicos para cada persona que vive con la enfermedad. Navegar por la EP implica crear un equipo de atención con especialistas que puedan atender los síntomas a medida que aparecen, crear una red de apoyo y mantenerse activo.
Encuentre clases de ejercicio y grupos de apoyo cercanos a través del Chapter más cercano de la Parkinson’s Foundation.
3 maneras de encontrar respuestas reales a preguntas acerca de la EP
- Para obtener respuestas inmediatas basadas en información y artículos de la Parkinson’s Foundation, pruebe nuestra nueva herramienta de chat impulsada por la IA, Ask PAM (Parkinson's Assistance Messenger, o mensajero de asistencia para el Parkinson). Pregúntele a PAM ahora.
- Llame a nuestra Línea de Ayuda al 1-800-4PD-INFO (1-800-473-4636), opción 3 para español, para hablar con un especialista en información y obtener respuestas personalizadas.
- Explore Parkinson.org/Espanol para obtener recursos e información personalizados acerca de los temas relacionados con la EP que más le interesan en este momento.
La misión de la Parkinson’s Foundation de ayudar a las personas a vivir mejor con Parkinson permanece fuerte todo el año. Estas son algunas formas en las que puede ayudarnos a generar conciencia acerca de la EP ahora mismo:
- Síganos en redes sociales.
- Inspire a otros con su Mi Historia con EP
- Inscríbase para los correos electrónicos de la Parkinson's Foundation.
- Encuentre un evento virtual o presencial cerca de usted.
Obtenga más respuestas y ayúdenos a generar conciencia acerca del Parkinson en nuestra página encuentre respuestas reales.