Symptom Management: Is it PD, Medication or Aging?

Shakiness, slowness and stiffness – key Parkinson’s disease (PD) motor symptom challenges – can be frustrating. Your PD doctor and other PD healthcare experts, such as an occupational therapist (OT), can offer management strategies to ease movement difficulties. Addressing movement issues early can keep you living your best life.
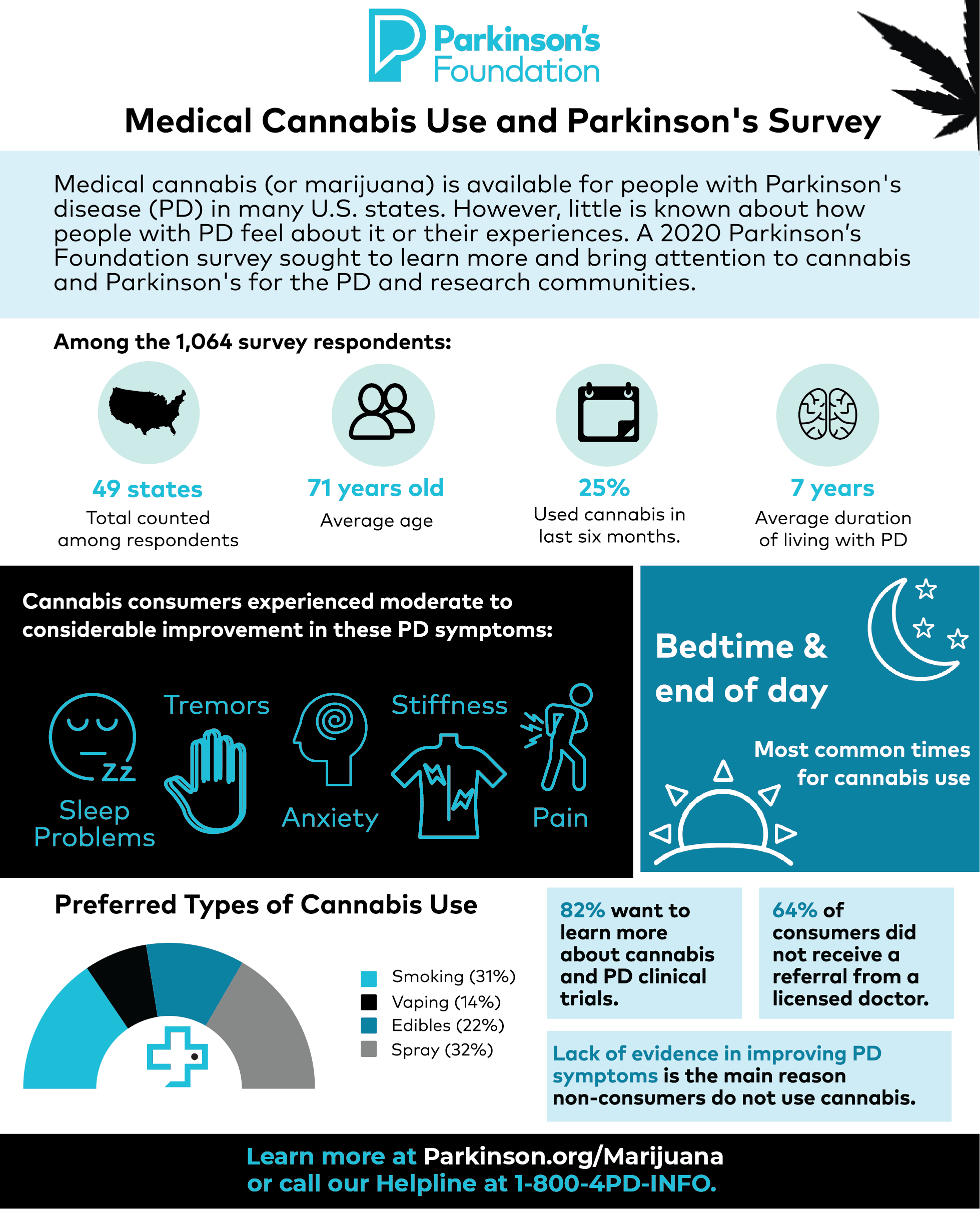
This article is based on a Parkinson’s Foundation Expert Briefing series on Symptom Management: Is it PD, Medication or Aging? “Exploring Motor Symptoms Co-Management: Occupational Therapy and Neurology” was presented by Lisa Warren, MHS, OTR/L, Occupational Therapist and Rehabilitation Manager, University of Florida Health Rehab, Norman Fixel Institute for Neurological Diseases, a Parkinson’s Foundation Center of Excellence; Parkinson’s Foundation National Medical Advisor Dr. Michael S. Okun, Adelaide Lackner Professor, Chair of Neurology and Executive Director Norman Fixel Institute; and Gretchen Rosswurm, 2020 Chair of the Parkinson's Foundation People with Parkinson's Council.
Cardinal PD Motor Symptoms
While there is no specific test to identify Parkinson’s disease, there are telltale primary – or cardinal – motor signs. These include:
- bradykinesia, the medical term for slowness of movement.
- tremor, or shakiness.
- rigidity and stiffness.
- postural instability or balance changes.
These symptoms stem from a drop in the brain’s production of the chemical dopamine. When considering a PD diagnosis, a neurologist who has PD expertise looks for bradykinesia accompanied by either stiffness or tremor.
Co-Managing Movement Issues
Both your neurologist and occupational therapist use different methods to tackle motor difficulties. Integrating multidisciplinary movement therapies can help you move easier.
Bradykinesia
We all tend to move a bit more slowly as we age. Bradykinesia – PD-associated physical slowness – is more unpredictable and exaggerated than typical age-related slowness. It can manifest as difficulty initiating movement. Or you may experience unusual stillness, decreased facial expression or need more time to complete daily tasks.
Your doctor may review the medications you are taking to ensure optimal delivery or might recommend taking your medications up to an hour before tasks that require dexterity.
An occupational therapist may recommend allowing extra time to accomplish tasks or can suggest activities that boost dexterity, such as shuffling and dealing cards. And remember, it’s OK to choose accuracy over speed. Give yourself permission to take the time you need.
The formula to living well with Parkinson’s is different for everyone. Be flexible and commit to working with your healthcare team to discover what works for you.
Tremor
People who live with Parkinson’s generally experience tremor as a shaky hands, legs or chin, often occurring at rest. Tremor typically affects one side of the body. Severity can fluctuate throughout the day – and from day to day.
Doctors often treat resting tremor with combination carbidopa/levodopa medication therapy. This temporarily replenishes dopamine to ease movement. But more than 20 percent of people living with PD can experience medication-resistant tremor. In these cases, a movement disorder specialist can recommend other therapies, including deep brain stimulation (DBS) – a procedure where electrodes are implanted into certain areas of the brain and connected to an implanted pulse generator to block nerve signals that make movement difficult.
Emotional and physical stress can also increase tremors. An occupational therapist can recommend therapies to combat your specific triggers – from meditation and creating a comfortable sleeping environment to adapting a favorite hobby.
Check out the PD Health @ Home online program called Mindfulness Mondays to discover ways to decompress.
Rigidity
This PD-related stiffness can occur throughout the body. Rigidity may cause painful cramping, such as dystonia – muscle spasms and clenching associated with Parkinson’s. Stiffness can occur on one or both sides of the body.
One of the best things you can do to combat rigidity is to take your medication on time, every time. If that isn’t working, your doctor may augment your medications or consider Botulinum toxin injections, which can sometimes relax overactive muscles.
Stress management and regular exercise can also ease rigidity and improve many other symptoms of Parkinson’s. An occupational therapist can recommend stretches specific to your needs. Warm up, then stretch your muscles before putting them to work. Be sure to talk to your doctor before starting any new exercise.
Stretch frequently, minimize stress and consider practicing yoga. The Parkinson’s Foundation offers online PD Health @Home Fitness Fridays to help you stay active at home.
Postural Instability
It's important to remain active with Parkinson's. However, people who live with PD can experience balance changes that increase the risk for falls and injury. Your healthcare team can give you strategies to keep moving safely.
Your movement disorder neurologist should perform a balance test that involves your shoulders at every visit. Your reaction to the test helps your doctor determine instability issues and potential treatment.
Integrate early, consistent, year-round physical and occupational therapy and exercise that focuses on balance. Ensure your home is free of clutter. Make it safe and easy to navigate. Minimize multitasking when you are walking; focus on walking and moving safely. Take big steps and walk with confidence.
Explore the Parkinson’s Foundation publication Fitness Counts to learn posture and balance tips and safe ways to get up from a fall.
Find Expert Care
Call the Parkinson's Foundation Helpline at 1-800-4PD-INFO (1-800-473-4636) or Helpline@Parkinson.org to find skilled Parkinson’s healthcare – including occupational, physical and speech therapy – in your area.
Related Blog Posts