Engaging the Parkinson’s Community in Research: The Path to Better Treatments

PD community involvement in trial design outshines recent clinical trial outcomes
The role of people with Parkinson’s disease (PD) in shaping research has never been more critical than today. “People living with Parkinson’s are experts, they have the lived experience and should be engaged as equal partners in the drug development process,” said Evelyn Stevens, Parkinson’s Foundation Senior Director of Community Engagement.
One avenue of engagement is the Patient Engagement Council for Parkinson’s Research (PECPR). Established in 2021, the PECPR has worked to ensure that the Parkinson’s community has a seat at the table in drug development. A collaboration between UCB, the Parkinson’s Foundation, Parkinson’s UK, and five people living with Parkinson’s, the council believes patient insights should guide research priorities.
The goal of the PECPR was to engage those with PD in research and trial design, guiding development toward results that will most impact and benefit their lives. The council:
-
Developed a “playbook” for including people with Parkinson’s feedback, ensuring that medicines are designed to address what matters most to the PD community.
-
Prioritized accessibility and inclusivity in all stages of treatment research, so that treatments are developed with the wide diversity of the PD community in mind.
-
Advanced the field of disease-modifying therapies for PD, which seek to slow, stop, or even reverse the disease progression rather than simply treat its symptoms.
The council’s efforts were recognized when it won a 2024 Made with Patients award from the Patient Focused Medicines Development, underscoring the impact of patient-driven collaboration.
PECPR played a key role in shaping a recent clinical study called ORCHESTRA, testing the efficacy of the pharmaceutical company UCB’s drug, minzasolmin. Unfortunately, in December 2024, UCB announced the study did not meet its efficacy goals. Days later, another pharmaceutical company, Roche, announced similar results — their intravenous PD drug called prasinezumab also missed the primary endpoint, but suggests possible benefit in early-stage PD.
Both drugs were designed to slow the progression of PD by targeting a protein called alpha-synuclein normally found in the brain. When this protein is mishappen and builds up in the brain it disrupts brain function and leads to PD symptoms. Neither drug significantly slowed disease progression in trial participants when compared to the participant group that received a placebo.
“Developing effective disease-modifying PD treatments comes with numerous challenges,” said Maggie Caulfield, PhD, Director of Research at the Parkinson’s Foundation. “One concern is that a therapy needs to reach the right area in the brain, get into the right cells, and interact with a particular molecule — all in a system where cells in the brain are already unhealthy.”
While the minzasolmin trial did not yield the hoped-for results, PECPR’s mission remains unchanged: to push for research that directly addresses the real needs of people with Parkinson’s.
Looking ahead, PECPR is focused on expanding patient engagement strategies, refining accessibility in research, and continuing to advocate for treatments that go beyond symptom management to fundamentally change the course of Parkinson’s.
Strengthening the Odds of Finding New Disease Modifying Therapies
While trial failures for disease modifying therapies for PD are disappointing, they ultimately provide researchers with new, valuable data that will guide the next round of treatments. Researchers can utilize data (positive and negative results) to help overcome previous biological hurdles.
“Parkinson’s researchers will keep trying and tweaking until we have the next breakthrough,” said Dr. Caulfield, “There are all kinds of different ways that researchers and clinicians are trying to reach disease related targets, we just have to keep pushing and eventually something will work.”
One area where patient engagement is vital is in genetics research. Understanding the genetic factors behind PD can help researchers develop more targeted, effective treatments. Pharmaceutical companies are already partnering with people with PD to improve their clinical trials that are based on genetic ties to PD.
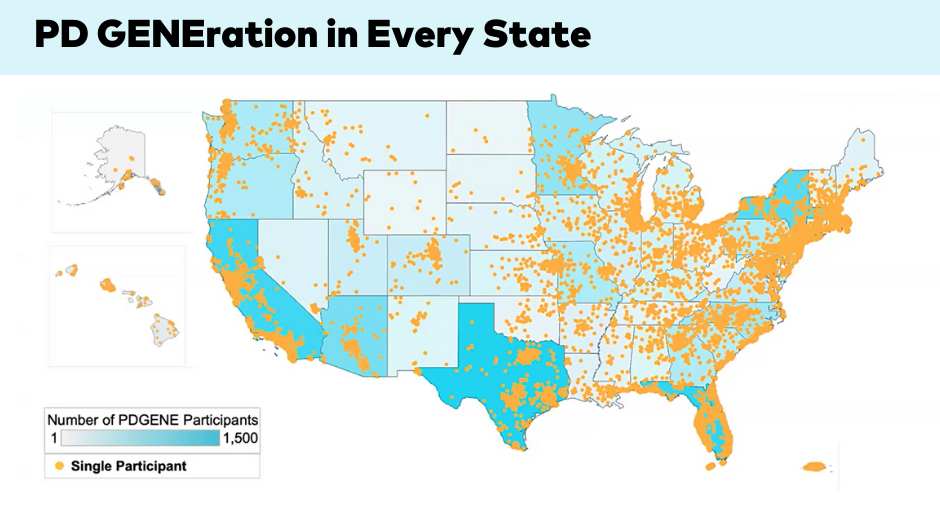
Studies like the Parkinson’s Foundation PD GENEration: Mapping the Future of Parkinson’s Disease are advancing this effort by offering free genetic testing and counseling to people with PD. By identifying genetic variants linked to PD, researchers can uncover new pathways for treatment — bringing the field closer to personalized medicine, where therapies can be tailored to a person’s genetic profile.
“There is a lot of hope in understanding Parkinson’s through genetics and leveraging study data to find the next disease modifying treatment,” said Evelyn.
Patience, Perseverance and Continued Progress
Every person with PD experiences unique symptoms and disease progression. These differences can be related to genetics, environment, age or other factors, all of which make finding new, effective disease-modifying therapies for PD a daunting task.
As PD research moves forward, the involvement of the PD community is invaluable and critical. Groups like PECPR and Parkinson’s Foundation research advocates ensure that the experiences of those with PD guide treatment development in ways most beneficial to the PD community.
“It’s an exciting time to see so many researchers and industry partners wanting to listen and learn from those living with Parkinson’s,” said Evelyn. “That’s what community engagement is all about — it’s a collaborative process where we combine our experience and expertise to improve the health of those living with Parkinson’s. That’s what will lead us to a cure for PD”
Learn More
The Parkinson’s Foundation works to improve care for people with PD and advance research toward a cure.
-
Discover how we are working to close gaps in knowledge about PD: Advancing Research
-
Learn about PD GENEration: our global genetics study that provides genetic testing and counseling at no cost for people with Parkinson’s.
-
Explore ways to get involved: from our research advocate program to joining a research study.
Related Materials
Pain in Parkinson's Disease
Occupational Therapy & Parkinson's
Nutrition and PD
Related Blog Posts

Visit the Parkinson’s Foundation Booth at WPC

Meet the Researcher Working to Develop an Imaging Biomarker for Parkinson’s