Un estudio demuestra que permanecer activo en el hospital beneficia a las personas con Parkinson

Las investigaciones demuestran que las personas con la enfermedad de Parkinson (EP) son hospitalizadas más a menudo, llegan a la sala de urgencias con más frecuencia y son más vulnerables a tener complicaciones durante su hospitalización.
El ejercicio y la actividad física no sólo ayudan a las personas con Parkinson a mantener o mejorar la movilidad, la flexibilidad y el equilibrio a la hora de controlar los síntomas, sino que el movimiento habitual puede ofrecer grandes beneficios en el hospital. Como paciente hospitalizado, el movimiento —a menudo con apoyo de fisioterapia y terapia ocupacional— es esencial para prevenir caídas y minimizar complicaciones.
Un nuevo estudio descubre que mantenerse activo (movilidad en el hospital) beneficia a las personas con Parkinson. Publicado en Parkinsonism & Related Disorders, el estudio apoyado por la Parkinson's Foundation examina cómo el Programa Move to Heal de los Hospitales Universitarios (UH, por sus siglas en inglés) ubicados en Cleveland, Ohio, un programa de movilidad en todo el sistema hospitalario que busca movilizar a todos los pacientes hospitalizados al menos tres veces al día, afecta a los pacientes con la EP.
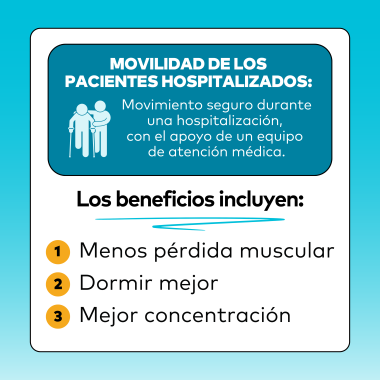
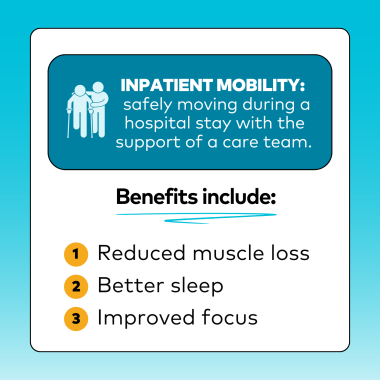
La movilidad de los pacientes hospitalizados se refiere al movimiento seguro durante la estancia en el hospital (dentro y fuera de la cama) con la aprobación y el apoyo de un equipo de atención médica. Los beneficios incluyen:
- Reducción de la pérdida muscular
- Dormir mejor
- Mejor concentración
La falta de movilidad de los pacientes de edad avanzada durante su hospitalización se asocia a una menor movilidad y a un aumento de la mortalidad tras el alta.
Resultados del estudio
Para aprender más acerca de los resultados de la movilidad hospitalaria para personas con la EP, el estudio utilizó datos de pacientes ingresados al hospital por más de 24 horas entre febrero y septiembre de 2023, comparando 300 pacientes hospitalizados con Parkinson con 12,000 pacientes sin la EP. Cada grupo se dividió a su vez en un:
- Grupo activo: tres o más movilizaciones al día. Las movilizaciones incluían rango de movimiento activo o pasivo realizado en la cama, sentado en el borde de la cama, sentado en una silla o en una silla retrete, de pie y caminando.
- Grupo inactivo: menos de tres movilizaciones al día.
Los datos mostraron que los pacientes hospitalizados con la EP del grupo activo tuvieron una estancia hospitalaria más corta y una mayor probabilidad de volver a casa tras la hospitalización. Esto apoya las Recomendaciones de atención hospitalaria de la Parkinson's Foundation, que promueve que las personas con la EP se movilicen tres veces al día bajo supervisión profesional.
En particular, todos los pacientes que permanecieron activos durante su hospitalización tuvieron un 50% menos de probabilidades de morir a los 30 días de recibir el alta hospitalaria y un 30% menos de probabilidades a los 90 días.

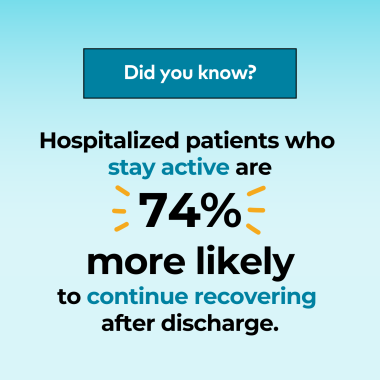
Los pacientes hospitalizados que se mantuvieron activos tuvieron un 74% menos de probabilidades de ser dados de alta para cuidados paliativos o de morir, en comparación con los pacientes inactivos.
En general, el estudio sugiere que la movilización frecuente disminuye significativamente la duración de la estancia y aumenta la probabilidad de ser dado de alta para volver a casa para los pacientes con Parkinson, en hospitales con programas de movilización.
Destacados
-
La Parkinson’s Foundation se asoció con los Hospitales Universitarios (UH, por sus siglas en inglés) para comprender mejor cómo afecta a las personas con Parkinson el hecho de permanecer activas en el hospital (lo que se denomina movilización de los pacientes).
-
Los datos del estudio compararon a 300 personas hospitalizadas con Parkinson con 12,000 pacientes hospitalizados sin Parkinson.
-
Las personas con Parkinson que fueron movilizadas al menos tres veces al día durante su ingreso tuvieron una estancia más corta y fueron dadas de alta para volver a casa (en lugar de a un centro asistencial) con más frecuencia que aquellas que no fueron movilizadas al menos tres veces al día.
-
Los pacientes que permanecieron activos durante su hospitalización tuvieron un 50% menos de probabilidades de morir a los 30 días de recibir el alta hospitalaria y un 30% menos de probabilidades a los 90 días.
-
Ambos grupos que estuvieron activos (con y sin la EP) tuvieron estancias hospitalarias más cortas que el grupo inactivo, pero el impacto fue más significativo para las personas con la EP.
-
Sólo el grupo de la EP activo mostró una mayor probabilidad de volver a casa tras el alta.
¿Qué significa esto?
Para las personas con Parkinson, mantener la movilidad en el hospital puede significar una enorme diferencia a la hora de recuperarse y tener más probabilidades de volver a casa en lugar de a otro centro asistencial.
La movilidad en las personas con Parkinson es un aspecto importante del manejo de los síntomas de la EP, tanto en casa como en el hospital. Este estudio demuestra que las personas con la EP tienden a experimentar estancias hospitalarias más largas y a tener mayores tasas de mortalidad si no se mueven con regularidad en el hospital.
Para muchos, puede resultar difícil promover un movimiento regular y programado cuando enfrentan problemas de salud o complicaciones que los llevan al hospital. Este estudio apoya los esfuerzos de la Parkinson's Foundation para promover programas de movilización de los pacientes hospitalizados en todo el sistema, mostrando beneficios significativos para los pacientes y los hospitales, especialmente aquellos con la EP. Con el tiempo, estos programas pueden ayudar a mejorar la calidad de la atención.

¿Qué significan estos hallazgos para las personas con la EP en este momento?
Cada año, más de 300,000 personas con Parkinson reciben atención en un hospital en los EE.UU. Sin embargo, se estima que aproximadamente una de cada seis personas con Parkinson experimenta complicaciones evitables durante una estancia hospitalaria.
No obstante, hay muchas formas de defenderse cuando se prepara para una estancia hospitalaria o la experimenta. La Guía de seguridad hospitalaria contiene herramientas e información útiles para ayudarle durante su próxima visita. Esta guía destaca cinco necesidades de atención hospitalaria, con consejos sobre cómo hablar con el equipo de atención acerca del movimiento dentro del hospital y posteriormente.
Aprenda más
La Parkinson’s Foundation cree en el empoderamiento de la comunidad de Parkinson a través de la educación. Aprenda más acerca de la EP y la movilidad en nuestros recursos mencionados abajo o llame a nuestra Línea de Ayuda gratuita al 1-800-4PD-INFO (1- 800- 473-4636), opción 3 para español, para obtener respuestas a sus preguntas acerca del Parkinson.