Parkinson’s Foundation Announces COVID-19 Survey Results
Survey measures how the Parkinson’s disease community is coping with the pandemic
MIAMI & NEW YORK (January 21, 2021) — The Parkinson’s Foundation today announced the results of a survey measuring how people with Parkinson’s disease (PD) are coping during the COVID-19 pandemic. The Parkinson’s Foundation collaborated with the Movement Disorders Division of the Department of Neurology at Columbia University Vagelos College of Physicians and Surgeons and the NewYork-Presbyterian/Columbia University Irving Medical Center to administer the survey. The goal is to provide guidance to clinicians, policy makers and the PD community on how COVID-19 has transformed the lives of people with Parkinson’s and their access to care.
“During these unprecedented times, this survey helps us better understand how we can support the PD community and meet their needs as the pandemic continues to impact their health and wellbeing,” said John L. Lehr, President and Chief Executive Officer of the Parkinson’s Foundation. “This survey further validates our mission to make life better for people with Parkinson’s disease and ensure they have access to the resources and information they need from the comfort and safety of their homes.”
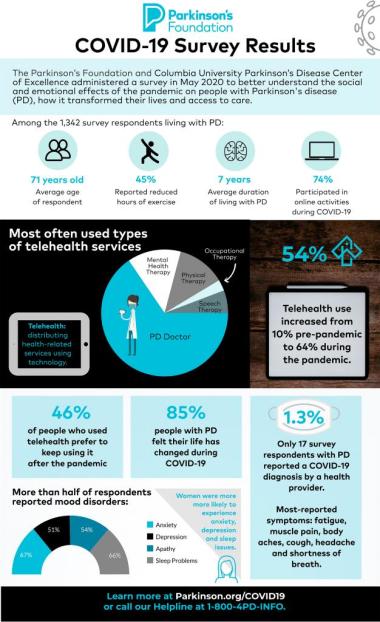
The survey, distributed in May 2020, focused on the health status, emotional health, attitudes and practices related to changes in the routines of people with Parkinson’s disease since the pandemic started. Only 1.3 percent of respondents with PD reported a COVID-19 diagnosis by a health provider while 38.5 percent were greatly concerned that they would become infected and require intensive hospital care. Similarly, 67 percent of respondents experienced nervousness or anxiety overall, 51 percent reported feeling down or depressed and 66 percent reported sleep disturbances. Women were more likely to experience these symptoms than men, with the exception of experiencing a reduced interest or pleasure in doing things.
The Parkinson’s disease and COVID-19 survey is the first to measure the use of telehealth services for people with PD during the pandemic. Telehealth use among the respondents increased from 10 percent prior to the pandemic to 64 percent during the pandemic. Those with higher income and higher education were associated with greater telehealth use. People used telehealth most often for a doctor’s appointment compared to other health therapies (mental health, physical therapy, occupational therapy and speech and language pathology). Among those who had used telemedicine services, 46 percent preferred to continue using telehealth always or sometimes after the COVID-19 outbreak ends.
“There is little doubt that the stress from COVID-19 and the limitations of social distancing affect everyone negatively, including people with PD. The survey highlights PD-specific issues and potential coping mechanisms, including online social support and telemedicine to reduce the burden caused by the pandemic,” said Roy Alcalay, MD, MS, the Alfred and Minnie Bressler Associate Professor of Neurology (in the Taub Institute) at Columbia University Vagelos College of Physicians and Surgeons and associate attending neurologist at NewYork-Presbyterian/Columbia University Irving Medical Center and survey lead. “The survey findings support that remote medical care can be very useful in these times and may be helpful to people with PD even after the resolution of the pandemic.”
The data from the survey strongly suggests disparities across socioeconomic status in people with PD during the COVID-19 pandemic, with those of lower income far more affected by financial and employment uncertainties. Factors such as location and local COVID-19 rates were not associated with mood symptoms. This suggests that communities deemed at lower risk of spread are not immune to the overwhelming influence of the COVID-19 pandemic on everyday life.
The Parkinson’s and COVID-19 survey, administered between May 2020 and June 2020, received 1,342 completed responses from people with PD. Respondents live across states that experienced all levels of COVID-19 infection. The average age for respondents was 71, and the average time they have lived with Parkinson’s was seven years. See the complete results of the study in the open access journal npj Parkinson’s Disease, the official journal of the Parkinson’s Foundation, created as part of the its commitment to share the latest Parkinson’s findings with the broader PD community.
Learn more about Parkinson’s and COVID-19 at Parkinson.org/COVID19 or by calling the Parkinson’s Foundation’s free Helpline at 1-800-4PD-INFO (473-4636).
###
About the Parkinson’s Foundation
The Parkinson’s Foundation makes life better for people with Parkinson’s disease by improving care and advancing research toward a cure. In everything we do, we build on the energy, experience and passion of our global Parkinson’s community. Since 1957, the Parkinson’s Foundation has invested more than $400 million in Parkinson’s research and clinical care. Connect with us on Parkinson.org, Facebook, Twitter, Instagram or call (800) 4PD-INFO (473-4636).
About Parkinson’s Disease
Affecting an estimated one million Americans and 10 million worldwide, Parkinson’s disease is the second-most common neurodegenerative disease after Alzheimer’s and is the 14th-leading cause of death in the U.S. It is associated with a progressive loss of motor control (e.g., shaking or tremor at rest and lack of facial expression), as well as non-motor symptoms (e.g., depression and anxiety). There is no cure for Parkinson’s and 60,000 new cases are diagnosed each year in the U.S. alone.